MAY 2019
Tick-borne diseases on the rise, but often misdiagnosed, underreported
Scott Heiberger
Communications Manager, National Farm Medicine Center
 Ticks were so plentiful on our overgrown campsite in Sawyer County, Wis., that a daily source of entertainment was to burn out the imbedded critters. My high school buddies and I would hold a match close, and watch all eight legs scramble in reverse as the tick tried to save his fast-blackening behind.
Ticks were so plentiful on our overgrown campsite in Sawyer County, Wis., that a daily source of entertainment was to burn out the imbedded critters. My high school buddies and I would hold a match close, and watch all eight legs scramble in reverse as the tick tried to save his fast-blackening behind.
Come to find out, applying heat to an infected tick can actually increase pathogen transmission by increasing its saliva production. You’re supposed to remove it with tweezers.
Although the fire ritual gave us a measure of satisfaction, a black-legged (deer) tick exacted revenge upon me years later in my central Wisconsin yard. I didn’t realize I’d been infected with Lyme disease until I endured a week of fevers, body aches, extreme fatigue and almost debilitating headaches, followed by another few days of simmering fever and the emergence on my trunk and limbs of two dozen pink, oval lesions with clear centers.
I received plenty of clues. I just couldn’t string them together. Neither could the nurse practitioner who thought I had the flu. In fact, the disease had reached Stage 2, in which the corkscrew-shaped Borrelia burgdorferi bacteria disseminated in my bloodstream, causing the lesions.
When I went back to the medical office a few days later, the doctor immediately said: “you’ve got Lyme disease.” He prescribed the antibiotic doxycycline. I felt better within 48 hours. Antibiotics are extremely effective when used early. If untreated, Lyme can cause serious neurological, heart and joint problems. Unfortunately, some people report chronic, lasting symptoms, even with treatment.
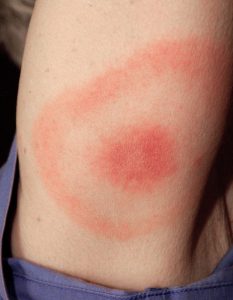
Classic “bulls-eye” pattern.
My biggest mistake was to miss the significance of the initial rash, which develops in up to 90 percent of Lyme cases. I noticed the rash one morning after sleeping in our yard, inside a zippered tent that had been stored in the house. The rash was not the classic “Bull’s-eye” Lyme rash you hear about. I figured something must have bitten me overnight, perhaps a spider in the bedding.
In reality, the rash was caused by a deer tick that had bitten me some days earlier. By the time I sought initial medical attention the rash was long gone, and I didn’t bother to mention it. Experts say Lyme disease can be difficult to diagnose because symptoms, including the rash, are not consistent and may imitate other conditions.
I wasn’t thinking Lyme. It was October and I assumed ticks were a spring and summer threat. Also, I had not ventured into woods recently, and wrongly believed that made me less vulnerable. Plus, most ticks I’d seen had been wood ticks, which do not carry Lyme.
But anyone in the Upper Midwest who spends time outside and becomes symptomatic should consider Lyme, or the other tick-borne diseases.
Lyme disease is the most commonly reported vector-borne illness in the United States, and the sixth-most common nationally notifiable disease.
There were nearly 30,000 confirmed cases in the United States in 2017, but Lyme is notoriously under-reported, and it is estimated that 10 times that number of Americans may have actually been diagnosed. (Lyme disease, CDC) Ninety-six percent of U.S. Lyme cases are concentrated in 14 states. Wisconsin (31.0 confirmed cases per 100,000 residents) and Minnesota (25.2 per 100,000) had the highest 2017 incidence rates outside the Northeast U.S.
Lyme disease and other tick-borne diseases (TBDs) are on the rise.
Even residents of urban areas are at risk, whether in parks or backyards, or when their recreational and occupational activities take them into the woods and grasslands of rural counties. It is speculated that warmer weather, forest regrowth and migration of deer into urban areas might explain the spread of tick-borne diseases. Children who spend time outdoors are especially at risk, as are adults with outdoor occupations. (Lyme Disease, Mayo Clinic)
The deer tick prefers mice and deer as hosts, but will settle for humans and other animals when a blood meal is needed. The bacterium is transmitted during the bite and blood draw, a process that can take 24-48 hours. The bacterium usually enters the victim late in the process. Not all deer ticks are infected with the bacterium that causes Lyme disease, and only an infected tick can transmit the disease. Early symptoms of infection mimic the flu – headaches, chills, nausea, fever, aching joints and fatigue. In approximately 70-80 percent of cases there is a bull’s-eye shaped rash at the bite site, which appears 3-30 days after the bite. (Lyme Disease, CDC)
Identification of effective methods to prevent Lyme disease has proven challenging. Measures aimed at reducing tick populations on residential properties have not proven effective in decreasing the number of human Lyme disease infections. (CDC MMWR). Long recommended behavioral interventions, such as wearing permethrin-treated clothing or using repellent containing DEET, have not been adequate to control Lyme disease on a population scale. (Middleton, Cooper & Rott, 2016) In addition, adherence to recommendations aimed at preventing Lyme disease has been poor, even amongst those who had previously suffered Lyme disease, precautionary measures remained unpopular. (Marcu et al., 2013) Even when adopted, most personal preventative measures are not highly effective. (Vazquez et al., 2008)
So if messages encouraging avoidance of habitat, use of DEET and tucking pant legs into socks are falling on deaf ears, then a simple, daily visual check for ticks on the body can be an effective way to prevent Lyme disease. Due to the amount of time required for B. burgdorferi to transit from the midgut to the salivary glands of the tick and into a new host, if ticks can be detected and removed before 36 hours of attachment, transmission of B. burgdorferi can effectively be prevented. (Clark & Hu, 2011).
Bottom line?
Check yourself, your family and your pets after being outside in non-winter months. It’s no fun – and potentially serious — when you’re the one who gets burned by a tick.
Scott Heiberger is a Communications Manager at the National Farm Medicine Center at the Marshfield Clinic in Marshfield, Wisconsin. He is the managing editor for the peer-reviewed Journal of Agromedicine and his a member of the UMASH outreach team.
